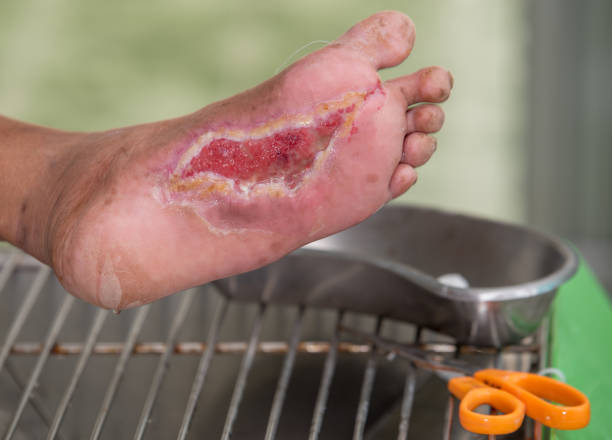
Key Takeaways
- Osteomyelitis is a bone infection.
- It can be sudden (acute) or long-standing (chronic).
- Treatment usually includes antibiotics and sometimes surgery.
- Physiotherapy helps people recover strength, motion and function after an infection or operation.
- This article explains the causes, how to spot the condition, treatment options, and how physiotherapy can help with recovery.
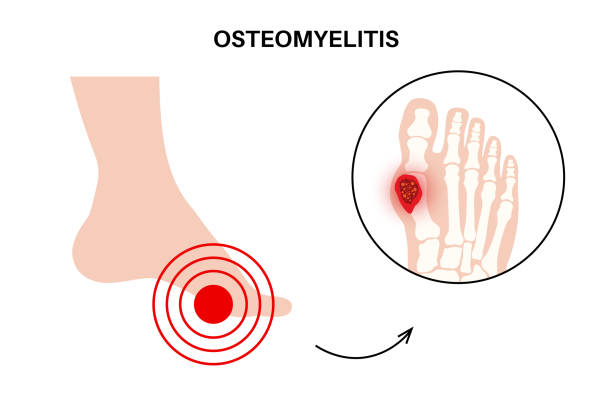
What is Osteomyelitis?
Osteomyelitis is a medical term for a bone infection. It occurs when the bone and marrow become inflamed by invading germs, most often bacteria.
Osteomyelitis was coined from three Greek words: osteon (bone), myelo (marrow), and -itis (inflammation), by a surgeon, Nélaton, in the 1840s.
Osteomyelitis can affect people of all ages. It can start small, as an infection in the body or the blood, before spreading to the bone and causing this condition.
In children, osteomyelitis starts as a bloodstream infection (hematogenous) before spreading to long bones, like the femur (thigh bone) or tibia (leg bone).
Whereas in adults, hematogenous osteomyelitis is less common and often affects the spine. More commonly, adult cases of osteomyelitis follow injury/surgery or diabetic foot infections (contiguous spread).
Osteomyelitis is much more common in kids than in adults. Generally, the incidence rate is relatively low, affecting about 22 – 24 in 100,000 people each year in developed countries. But it is a serious condition when it occurs.
Osteomyelitis, if not treated promptly, can block the bone’s blood supply, causing patches of bone tissue to die (necrosis). Over time, the body may form new bone (involucrum) around the dead fragments (sequestrum).
Causes of Osteomyelitis
Staphylococcus aureus, a bacterium normally found on the skin and in the nose, is the most common cause of osteomyelitis.
Other bacteria can cause osteomyelitis too, including Streptococcus species, gram-negative organisms (like E. coli), and, in some chronic cases, Mycobacterium tuberculosis.
However, Staph. Aureus accounts for the majority of osteomyelitis cases.
How Does Infections Reach the Bone?
Osteomyelitis can occur when bacteria or other organisms enter the bone through various routes. The main routes are:
- Through the blood – Hematogenous spread: This is when bacteria travel in the bloodstream from another site (eg, a skin or lung infection) and settle in the bone. This is more common in children.
- From nearby tissue – Contiguous spread: Infection from nearby tissues, like a skin ulcer or open wound near a bone, spreads into the bone. This often happens in adults with diabetic foot ulcers or pressure sores.
- Direct entry – Inoculation: Occurs when an open fracture or surgery with a contaminated orthotic device introduces bacteria directly into the bone.
Types of Osteomyelitis
Osteomyelitis is often classified based on how long it has been present:
- Acute Osteomyelitis:
This is when the infection is still in its early phase (usually within the first 2 weeks). There is no significant bone death yet. Patients with osteomyelitis in the acute stage often come down with sudden high fever and intense bone pain. Prompt treatment at this stage usually leads to a good recovery.
- Subacute Osteomyelitis:
This is somewhat an in-between stage (2 – 8 weeks). Patients in this stage have a modest pain level and lower-grade fever.
- Chronic Osteomyelitis:
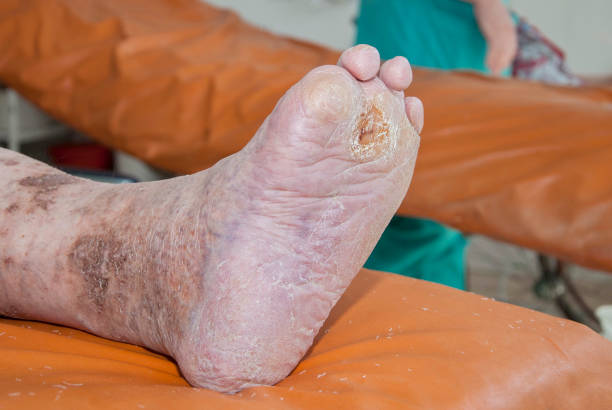
This is the long-standing stage of the infection and is typically defined as lasting longer than about 3 months or with visible dead bone on imaging. Patients with osteomyelitis in the chronic stage often develop dead bone pieces (sequestra) and draining sinus tracts in the affected areas. Chronic osteomyelitis is harder to treat and frequently reoccurs.
How Osteomyelitis Develops
This is what the sequence of events in osteomyelitis looks like:
- Bacteria get into the bone. It can be through the bloodstream, injury, or from a nearby infected tissue.
- The body’s immune system sends white blood cells to fight the bone infection.
- As white blood cells attack the infection, they also release enzymes and toxins that damage infected bone tissue, and in some cases, surrounding healthy bone tissue.
- This forms pus (a thick collection of dead cells and bacteria), which raises the pressure inside the bone.
- This built-up pressure affects tiny blood vessels, cutting off the bone’s blood supply.
- Without blood, parts of the bone tissue die. This is also called necrosis.
- As the affected bone dies, it separates from the healthy bone, forming pieces called sequestra.
- These sequestra can hold bacteria, shielding them from antibiotics.
- As a defense response, the periosteum (bone’s outer covering) lays down new bone around the sequestra. This new shell is called an involucrum.
- Over time, the pus and dead material may find a way out.
- They can form a channel through soft tissues to the skin, creating a sinus tract that drains pus.
- Sinus tracts are a hallmark of chronic osteomyelitis.
This cycle of infection → inflammation → dead bone → new bone explains why osteomyelitis can become self-sustaining and hard to eradicate without removing the dead bone.
Who is at Higher Risk?
Although anyone can get osteomyelitis, certain factors can greatly increase your risk of having osteomyelitis. These factors/conditions include:
- Fractures or bone surgery
- Implants or prosthetic devices like artificial joints or metal rods
- Poorly controlled diabetes mellitus
- Blood disorders that cause poor circulation, e.g., peripheral vascular disease
- Sickle cell disease
- Immunosuppression from long-term steroid therapy, chemotherapy, or conditions like HIV/AIDS or cancer
- IV drug use
- Chronic ulcers or pressure sores
- Children and older adults
If you fall into these groups and have persistent bone pain or wound problems, see a doctor immediately.
Common Symptoms (What to Watch Out For)
- Deep, persistent bone pain. It often worsens with movement.
- Redness, warmth, and swelling over the bone
- Fever, chills, or fatigue
- Reduced use of the limb due to pain or stiffness. Children often refuse to use that limb.
Symptoms vary. Some people have only mild signs. If you have persistent pain with fever or a non-healing wound, again, seek medical care.
Also, in chronic osteomyelitis, you may notice a persistent draining wound (sinus tract) or discharge of pus over the bone. There could also be bone deformities and muscle wasting around the area.
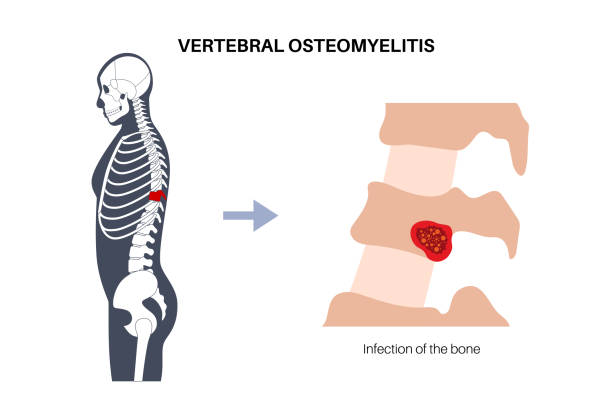
How Osteomyelitis is Diagnosed
- At the clinic or hospital, your doctor will get your full health history. They will likely ask about recent infections, surgeries, or wounds.
- Blood tests are often done, and if your inflammatory markers (CRP, ESR) are raised, it often points to an infection, however, it is not specific.
- In some cases, a bone biopsy or culture may be done to identify the exact germ causing the condition and to guide your health practitioner in prescribing antibiotics.
- Imaging, like X-ray, CT, or ultrasound scan can be performed to detect early bone infection and soft tissue involvement. If initial X-rays are normal but suspicion remains high, advanced imaging like MRI can be done. MRI is the most sensitive test for early infection.
Treatment of Osteomyelitis
- Long courses of antibiotics lasting several weeks are common. Typically ~4 weeks for children with acute hematogenous osteomyelitis and 6 – 8 weeks for adults/chronic cases. It can be IV or oral antibiotics.
- In chronic osteomyelitis or when there is a dead bone (sequestrum), surgery is often needed to remove infected tissue. This also allows antibiotics to reach healthy bone more effectively.
- Your doctors will monitor symptoms and repeat lab tests and imaging as needed.
- Alongside antibiotics, you need good nutrition, pain control, and should manage chronic conditions like diabetes, if you have them. If you are on any prosthetic devices or hardware that are loose or infected, you may need to have them removed or replaced.
Treating osteomyelitis takes time. You may go weeks on antibiotics or take months to fully recover.
Physiotherapy: What it is and Why it Matters
Physiotherapy cannot cure the infection, but it is crucial once the infection is under control. It is not a substitute for antibiotics or surgery. Instead, physiotherapy helps with recovery goals. So if you have:
- Pain and swelling
- Reduced joint range of motion (ROM) near the affected bone
- Muscle loss
- Reduced strength
- Impaired walking and difficulty performing daily tasks safely
Physiotherapy can help manage these signs and symptoms, and prevent complications. Recent research has shown this, especially when started early. Ideally, you shouldn’t start physio for this condition independently without getting the necessary clearance from your medical team.
Safety Signals During Rehab
Whether you’re at the clinic, with your PT, or doing home programs, call the attention of your physiotherapist or health personnel if you notice any of these:
- Increasing or sharp bone pain
- New fever, chills, night sweats
- New or worsening redness, swelling, or wound drainage
- Sudden weakness or loss of function
These signs can indicate that the infection is still active or that your treatment needs review.
General Tips for Osteomyelitis Patients
- Follow the full antibiotic course exactly as prescribed. Never stop antibiotics early, even if you feel better. Completing the entire course is essential to prevent relapse
- Keep wounds and dressings clean and dry.
- Start rehabilitation slowly. Don’t push your body to break all limits in one day. Small progress every day is normal.
- Ask for clear home-exercise instructions. If you don’t understand, relate to the team.
- Keep appointments for labs or imaging, so your team can track recovery.
How Long will Recovery Take?
Antibiotics alone often continue for 4 – 6 weeks or longer. Full recovery of strength and function can take weeks to months, depending on the severity of the infection and whether surgery was needed. Overall, be patient and follow your rehab plan.
When to Get Urgent Help
Go to emergency care if you develop:
- High fever with severe bone pain
- Rapid swelling or pus from a wound
- Confusion, fainting, fast heartbeat, or very low blood pressure
These may be signs of severe infection or sepsis.
FAQs on Osteomyelitis
No. When your treatment and rehabilitation are directed by a qualified physiotherapist in coordination with your medical team, your infection won’t get worse. Relapses can happen due to re-exposure to the bacteria or a repeat infection from an infected bone to another area.
Yes, in some cases you will need surgery for osteomyelitis. Surgery is needed if antibiotics alone cannot clear the dead bone or an abscess.
Yes, you need a clear program from your therapist to exercise at home. Most importantly, avoid pushing through severe pain when exercising.